Welcome to the Neurexpert Blog
Translating the Latest Neuroscience Research.
What connects schizophrenia and autism?
by Carolyn Lacey , 12 Oct 2015.
The common brain
On the surface, many brain disorders appear to be quite different.
It’s not often that you hear of someone with, say, depression being compared to someone with schizophrenia or, indeed, Autism Spectrum Disorder (autism).
However, if you dig deeper and break down the symptoms you will find that they share some commonalities: altered social interaction; impaired cognitive function; memory impairment; tendency towards compulsive behavior; attention deficits; and abnormal sensory processing.
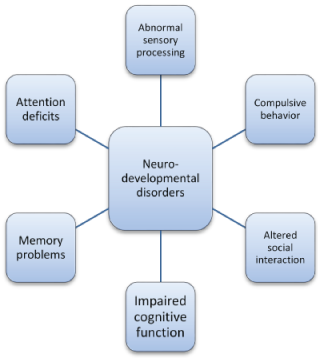
This doesn’t mean that those disorders are the same. It’s just that the brain is limited to how it expresses functional problems by its architecture and its building blocks.
When similar brain areas and the connections between those areas are disrupted it can result in similar detours of function.
The findings that I am going to present to you today are from a recent study published in Molecular Psychiatry by researchers led by Marga Behrens in the lab of Terry Sejnowski at Salk Institute for Biological Studies, La Jolla, CA, USA., in collaboration with Athina Markou's lab at University of California, San Diego (UCSD) CA, USA.
I am going to tell you about how they used genetic engineering in mice to produce brain changes and behaviors like those seen in neurodevelopmental disorders, such as schizophrenia and autism.
We are going to cover some brain basics before moving on to the current research.
The brain map
The brain is divided into different areas that have different functions. In order for us to properly navigate the world, these brain areas need to communicate with each other.
I like to think of the brain as having a system of cities (brain areas) and roads connecting the cities.
Brain cells, called neurons, reside within the cities and they carry information to other neurons with an axon that forms the “road”.
Neuron roads can be split into two broad categories:
- those that cross borders into other brain cities (projection neurons)
- those that like to stay more local and within the limits of their borders (interneurons)
Balancing the brainways
Neurons talk to each other with neurochemicals, sensors of neurochemicals (called receptors) and electrical activity, passing information via connections (called synapses) at the end of their road.
The projection cells tend to be drivers of activity (excite), containing a neurochemical called glutamate that causes cells to generate electrical impulses.
The interneurons, on the other hand, tend to contain neurochemicals that put the brakes on activity (inhibit), containing a neurochemical called GABA that prevents cells from generating electrical impulses.
Here’s where it gets a little mind-boggling. Because these two types of cells have to talk and need to be controlled, receptors for both types of neurochemicals are located on both cell types.
There are glutamate (drivers) and GABA (brakes) receptors on projection cells and interneurons. These receptors allow cells to be excited (driven) and inhibited (brakes).
It is thought that the brain needs these two systems to be “balanced” in order to function properly. A tip in the balance towards more or less of either one can derail normal brain communication.
Thus, as a way of controlling the balance, many pharmaceuticals developed for treatment of brain disorders target receptors.
Brain engineering
What if I told you that deleting one gene that controls one brain receptor can cause brain and behavior changes associated with neurodevelopmental disorders, such as schizophrenia or autism? And, also, that this effect can be created by deleting that gene, not from the entire brain, but, from just one subtype of brain cell?
And not only that…
What if I told you that the gene doesn’t have to be deleted from day one of development? But can be deleted after birth… at a specific point in time… and still cause neurodevelopmental disorders?
The Salk researchers did just that. They engineered a mouse that enabled them to delete a single type of neurochemical receptor on a single type of neuron at a chosen point in time after birth (but while the brain is still developing).
Here are the two things you need to remember to follow the results. This paper is about:
- A type of local inhibiting interneuron called parvalbumin cell (contains GABA)
- A type of driving receptor called mGluR5 (responds to glutamate)
Detours from normal function of both have been linked to neurodevelopmental disorders.
Connecting engineering to behavior
Although mGluR5 is located on many kinds of brain cells, the researchers used a type of genetic engineering technology that made it possible to remove mGluR5 only from the parvalbumin cells.
mGluR5 was deleted from parvalbumin cells in the cortex (recognition memory, sensory processing) and the striatum (motor habit, compulsivity, addiction). Thus, communication within each of these brain cities and communication through the roads connecting these cities was affected.
Because the above brain connections were affected, the engineered mice had symptoms similar to those seen in neurodevelopmental disorders, such as schizophrenia and autism:
- Recognition memory deficits. This is the ability to recognize previously met events, objects, or people (… or mice in the case of mice!)
- Heightened compulsive behaviors such as grooming and burying marbles
- They are more startled in response to a noise that they have been trained to ignore. Usually when rodents or people are trained to expect something startling with, say, a buzz, then they start to ignore the buzz… similar to riding in an elevator. When you hear a ping to tell you that you have arrived at your desired floor you are not startled by the doors opening. Translated this means that these engineered mice had problems with processing information from the sensory environment (outside world).
- Changes in the way they respond to drugs of abuse (amphetamine and PCP)
As mentioned earlier in the blog: the way that the brain displays output is restricted by the way it is built and the blocks (like receptors) used to build it. When similar brain cities, roads and blocks are disrupted, it can result in similar detours of function.
What contributed to behavior changes?
The behavioral changes observed in these mice are likely caused by a change in the influence of parvalbumin cells on brain activity (because of the deletion of mGluR5).
Removing mGluR5 from parvalbumin cells has been done before (see in reading list). It caused the mice to have neurodevelopmental deficits. However, the mGluR5 were deleted before conception and so the mice developed in utero with the receptor missing. The problem with this is that you don’t know how the brain might have compensated during development to control any problems that might occur due to the missing receptor. Because of this, cause and effect is harder to determine.
What makes the current study different is that they started deleting mGluR5 from parvalbumin cells two weeks after the mice were born. Any changes observed in these mice should, therefore, be less due to compensation and more due to the actual role of those receptors in those cells.
The Salk researchers found that, by 6 weeks old, the number of parvalbumin cells that contained mGluR5 was reduced by 65% in the engineered mice.
This means that: 1) the drive of parvalbumin cells through mGluR5 was reduced; 2) less drive of parvalbumin cells means less brake neurochemical GABA released onto other cells (including driver cells).
So, in all, you have less brake activity to balance out the drive activity. As I mentioned before, both systems need to be balanced in order for the brain to function properly. This shift in balance will lead to a change in the amount of electrical activity generated in the brain.
What about a biomarker for neurodevelopmental disorders?
Distinct, but complementary, brain areas communicate quickly over relatively large distances.
For instance, if a truck is moving towards you then brain areas associated with sound, vision and movement interact quickly in order for you first to be aware (attention) and then for you to respond (action).
Researchers have hypothesized that both schizophrenia and autism are fundamentally disorders of the brain’s ability to integrate complementary brain area information.
Brain cells in different cities “pulse” electrical activity in synchrony to create waves of activity known as oscillations. Gamma oscillations (frequency of 30 Hz to 100 Hz) help coordinate information created by neurons in distant brain areas.
This helps the brain perform more demanding tasks such as perception, attention, memory, and social interaction, amongst others.
The parvalbumin cells that were manipulated in this Salk study are important for generating and regulating gamma. Although the researchers didn’t observe any changes in brain oscillations in the engineered mice when the mice were just hanging out; when the mice were played a loud noise they saw an increase in gamma activity (greater than the increase in normal mice).
Both enhancement and reduction of gamma activity has been found in humans with neurodevelopmental disorders. In the case of schizophrenia, increases in gamma have been linked to so-called “positive” symptoms (such as auditory hallucinations) and decreases in gamma have been linked with so-called “negative” symptoms (such as social impairments).
Too little gamma could lead to a break down in brain communication and too much gamma may mean too much information is being transmitted (leading to, for instance, hallucinations).
Different mechanisms could underlie increases or decreases in gamma activity. Knowing the specific brain building blocks that regulates gamma could help develop targeted treatment for specific symptoms of neurodevelopmental disorders.
In fact, measuring changes in gamma activity could be a biomarker for identifying abnormal brain communication and neurodevelopmental disorders. You can measure brain oscillations from non-invasive wires on the scalp, or, directly from a brain in the lab/ clinical setting.
Studying Brain Oscillations
Brain oscillations are a fundamental feature of the networks of neurones in the brain. In patients with neurological or psychiatric disorders there is evidence that this activity is impaired. Recording this activity, with techniques such as EEG, may provide a biomarker of the disease.
When developing new medicines, scientists perform a wealth of experiments before they can test the potential new treatment in patients. Experiments studying gamma oscillations may therefore yield data that is 'translatable', meaning predictive of effects of new drugs on oscillatory activity in patients.
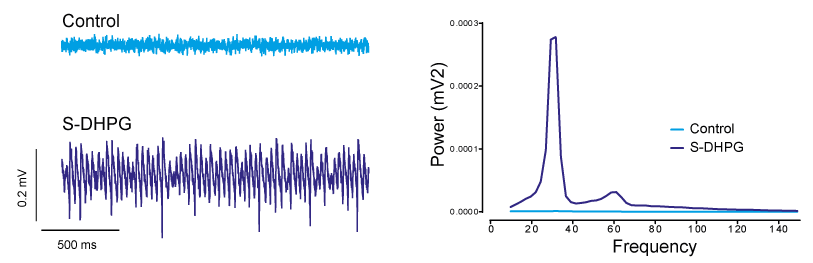
Oscillations can be induced in the laboratory by treating the network with certain chemicals. In the example above Neurexpert scientists treated the network with a compound called DHPG. This acts at the mGluR receptors discussed in this blog and results in the network oscillating in the gamma frequency. Further information on the use of oscillations and EEG can be found on our YouTube channel: http://www.youtube.com/watch?v=ZRgX1dH1pf8
The DHPG used in these experiments was kindly provided by hellobio. Click here for further information.
What does this study tell us about treatment of neurodevelopmental disorders, especially in children?
It is interesting that deletion of a single molecule on a single type of brain cell after birth can result in all of these behavioral changes in mice that are similar to those seen in neurodevelopmental disorders.
The key word here is development. In humans, the brain continues to develop through childhood and adolescence. As shown in this study, even after birth, changes to the brain can result in major changes in brain function and results in changes in behavior.
In everyday life, we interact with these developing brain circuits by the use of pharmaceutical agents to treat all kinds of neurological problems. Many of these pharmaceutical agents, while selective to receptor types, are not restricted to neuron type or brain area.
This study highlights how it may be important, especially in young humans, to develop pharmaceuticals that can act on specific receptors on specific brain cells, so that we do not inadvertently impact brain development in areas that might be working properly, and, so that we can target specific symptoms more effectively.
Conclusion
As mentioned in the beginning, many brain disorders have overlapping and common changes in behavior. These commonalities are not limited to schizophrenia and autism, but are found in other disorders such as Obsessive Compulsive Disorder, Tourette’s Syndrome, Attention Deficit Hyperactivity Disorder, depression and addiction, to name a few.
This is partly because the brain is limited by its building blocks and its connections.
Connections, and communication between these connections, drive behavior. In this case the cortex (recognition memory, sensory processing) and the striatum (motor habit, compulsivity, addiction) are the brain regions that are most affected.
Thus, even a small change in the brain’s building blocks can lead to functional and behavioral changes dictated by the brain areas affected. This means that symptoms of many neurodevelopmental disorders can have common and overlapping causes, even if they have different genetic and environmental factors at the root of each disorder.
To view the original paper discussed in this blog “Disruption of mGluR5 in parvalbumin-positive interneurons induces core features of neurodevelopmental disorders.” in Molecular Psychiatry please click here.
Further reading:
http://www.nature.com/mp/journal/v9/n1/full/4001404a.htmlhttp://journal.frontiersin.org/article/10.3389/fnins.2015.00086/full
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3595504
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3253230
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3361599/
http://www.psychiatrictimes.com
The Blog was written by Carolyn Lacey, Scientific Outreach Manager at Neurexpert. To learn more about Carolyn and Neurexpert, please click here.
Recent Blog Posts
Want to rid your brain of toxic build-up and perhaps stave off Alzheimer’s Disease? Don’t sleep sitting up
Planning on taking a power nap at your desk today? You might want to think twice about your sleeping position. The research article I’m about to summarize makes me think of all those times I have actually managed to get some sleep on a long-haul flight… only to wake up still feeling terrible (even after drinking litres of water) and all the elderly people I know who often like to take cat-naps sitting in their favorite armchairs.
What has birth got to do with autism?
A prominent neuroscientist suggests that the trend towards greater birth interventions could be correlated with greater incidence of autism spectrum disorders. We discuss his reasoning in our latest blog post.
Sleepless with the Enemy: how skipping sleep changes your social life and how dreams become reality
Ever stay up too late and wake up thinking the world is out to get you? We cover a new study that shows that sleeping and dreaming helps you read other people better. Skipping just one night of sleep makes your brain read threat in friendly faces and, in contrast, bigger dreams make for better reality.
Depressed? Suck it up!
Depression sucks and anti-depressants often don't work. Our latest blog sniffs out a new treatment published in Molecular Psychiatry that could be the future for #depression sufferers.
Stressed out of my mind
June 27th is Post-Traumatic Stress Disorder (PTSD) Awareness Day and so this blog is dedicated to neuroscience related to chronic stress.
Exciting times ahead at Neurexpert
Neurexpert appoints Dr Carolyn Lacey as Scientific Outreach Manager

Brochure Publications