Welcome to the Neurexpert Blog
Translating the Latest Neuroscience Research.
A trophy brain: the neuroscience of concussion in sports
by Carolyn
Lacey , 24 Nov 2015.
The dramatic side of brain injury
“Life's not about how hard of a hit you can give... it's about how many you can take, and still keep moving forward.” ― Sylvester Stallone as Rocky Balboa
Yo Adrian! The movie industry does an excellent job of glorifying Traumatic Brain Injury.
Knockout rounds with slowed down moments of fists hitting the jaw, sweat soaring high, the head twisting and turning, prior to the person falling to the ground. Those tantalizing quiet moments where the person is out cold, everyone in the crowd waiting, coaches holding their breath, only for the person to rise again and win.
How many times have we seen those themes in movies? The Rocky movie franchise thrived on these moments. Sylvester Stallone is even in the International Boxing Hall of Fame! If you Google “knockouts in movies” you will find lists with titles such as “TOP 10 GREATEST MOVIE KNOCKOUTS” and “15 Classic Bone-Crunching Movie Knockouts”. And it’s not limited to boxing movies. Plenty of genres, from Bond movies to children’s movies, Looney Toons or Tom and Jerry “seeing stars”, thrive on those moments where someone gets hit down and then gets back up to win.
But here’s some trivia: a knockout is a traumatic brain injury.
And: traumatic brain injury can have dire long-term consequences on your mental health.
- Rocky
- Cinderella Man
- Days of Thunder
- Back to the Future
- Raging Bull
- Snatch
- Uncle Buck
- Happy Gilmore
- Fight Club
- Warrior
- Any Given Sunday
- The Big Lebowski
- Peter Pan
Mild traumatic brain injury, or concussion, is when the brain rapidly moves in the skull, causing damage to the physical components of the brain that leads to neurological problems. In real life, more than 40 million people worldwide get concussions a year.
Concussions can tremendously alter quality of life with significant social, relationship and working/ school life challenges. The effects of concussions are dose-dependent, meaning that the more you endure the worse the outcome for your brain health. Another hit before full recovery can cause more severe and prolonged symptoms, and can even be fatal.
Youth have a much harder time recovering from concussions than adults as developing brains suffer greater injury severity, worse long-term outcomes and increased recovery time, with girls fairing worse than boys.
Multiple concussions, even when spaced years apart, pose risks of serious conditions, such as degenerative brain disorders like dementia (including Alzheimer’s Disease) and Parkinson’s disease, depression, and other long-term brain function deficits (post-concussive syndrome/ epilepsy/ headaches).
Concussion definition:
Head trauma resulting in loss of consciousness for less than 30 minutes; and/or alteration of mental state for up to 24 hours; and/or loss of memory for events surrounding the trauma. Loss of consciousness is not a requirement.
Sporting brains: raising awareness to the silent epidemic
“It's not necessarily the laws of the game that's the problem -- it's the awareness of the injury. It's more about players not trying to be heroes." – Jonathan Thomas, Rugby
Exercise and sports are extremely beneficial to brain health. The downside is that they tend to be high-impact. Brain injury is the number one cause of death in sport. In the US alone, 3.8 million cases of sport-related concussions occur annually. The incidence of concussion is highest in boxing, American football, soccer (particularly “heading” the ball), rugby and ice hockey.
Language of concussion:
- Confusion/ disorientation
- Headaches
- Nausea
- Cognitive slowing
- Fatigue
- Dizziness
- Sleep disturbance
- Speech impairment
- Attention and memory problems
- Can persist days to years
- You do not need to lose consciousness
But there’s good news: athletes of high-impact sports and the general public are now more aware of the effects of multiple concussions. Major sporting organizations such as National Football League (NFL), Major League Baseball (MLB) and World Rugby Organization (WRO), as well as school authorities, have been upping their game. There have been major changes to regulations to improve identification of concussion (such as video footage in medical rooms, and players wearing head-movement sensors as seen in NFL and NHL and recently adopted by the Saracens rugby club), removing players from games and prescribing rest so that the brain has time to recover.
"I don't want to be visiting these players in 20 or 25 years time in a hospital where they are suffering from dementia or some other neurological condition" – Ed Griffiths, Rugby
In Rugby, concussion occurs at a rate of about 1 in every 3 games (amongst all players involved; source Rugby Football Union). In the 2015 RBS Six Nations the Welsh rugby player George North was allowed to play on, despite suffering two concussions in one game against England (and a third later that rugby season). However, due to aggressive push to improve concussion management in Rugby, in the recent Rugby World Cup many players were taken off the field for suspected concussion. For example, Matt Giteau was taken out of the highly anticipated final between big rivals Australia and New Zealand after being knocked unconscious early in the game.
In milliseconds the brain can let you know that you have strained your groin, pulled your hamstring or broken a bone. It lets you know in the form of pain. The brain, however, does not communicate injury to itself with pain. Concussion is often referred to as the silent injury. It’s hard to see a concussion so diagnosis often requires the injured person to “own up” to their symptoms and seek help. However, at least a quarter of people who have a concussion do not seek hospital care.
Scientists are still researching how long the brain needs to recover from concussion. Each concussion is different and each person presents injury and recovery differently.
Even less is known about youth brains. Over half of sport-related concussions occur in youth under 19 years old with a doubling of emergency room visits in this age group the past decade (American Academy of Pediatrics).
However, concussions, unlike many brain disorders, have a known cause (head trauma) and, in the majority of cases, are preventable. The National Federation of State High School Associations (NFHS) has outlined “nine fundamentals for minimizing head impact exposure and concussion risk” (see box: Towards better sport concussion management).
Towards better sport concussion management
Many sport organizations have a new concussion protocol to follow during games. The World Rugby “Recognise and Remove” message incorporates 6 Rs: Recognize symptoms → Remove from play → Refer to a healthcare professional → Rest until symptom free → Recover (longer for kids) → Return when evaluated to be safe (Graduated Return to Play protocol). Source: World Rugby
National Federation of State High School Associations (NFHS) outline for minimizing concussions can be found here: https://www.nfhs.org/articles/concussion-task-force-recommendations-to-be-implemented-in-2015/
I am hoping to convince you in this blog that concussions are not great for your brain, your mental health and your longevity. However, if you do not want to read further then I have one take-home message: if you think that you have a concussion then do not be a hero. There is no glory in getting up and continuing to compete despite a traumatic brain injury.
Game over: multiple concussions can lead to dementia and depression
“Of all the things I’ve lost, I miss my mind the most.” - Mark Twain, author
It is becoming more apparent that the long-term brain health of athletes who compete in high-contact sports like boxing and American football can be compromised.
Athletes have been diagnosed with any, or all, of the following: cognitive ailments/ headaches (sometimes under the umbrella term: post-concussion syndrome), depression, and a special kind of dementia called Chronic Traumatic Encephalopathy (CTE; or, historically dementia puglilistica/ “punch drunk” syndrome).
Dementia?… that’s something only old people get… right?
Wrong.
It is not limited to older players, or professional athletes who made a career out of the sports; it’s also found in players at the beginning of their professional careers (as young as 18) and in those who haven’t played since they were teenagers. This is a dementia that can affect young and rising stars.
Although not all athletes develop dementia, there is one thing the diagnosed have in common: they all have history of multiple concussions.
It has been suggested that Muhammed Ali’s (boxing) Parkinsonism and Lou Gehrig’s (baseball) amyotrophic lateral sclerosis (ALS) may have links with multiple concussions. “Lou Gehrig’s Disease” is even a name synonymous with ALS.
Athletes with neurological disorders possibly linked to concussion:
- Muhammed Ali - Boxing; parkinsonism
- Lou Gehrig - Baseball; ALS
- Jonathan Thomas - Rugby; epilepsy
- Fred McNeill - American Football; CTE
- Abby Wambach - Soccer; post-concussion syndrome
- Dave Scatchard - Ice Hockey; post-concussion syndrome
- Terry Long - American Football; depression/ suicide age 45
- John Jaso - Baseball; migraines/ depression
- Junior Seau - American football; CTE, suicide age 43
- Cindy Parlow Cone - Soccer; post-concussion syndrome
- Patrick Grange - Soccer; CTE with ALS age 29
- Ryan Freel - Baseball; CTE, Suicide age 36
- Shontayne Hape - Rugby; migraines/ depression/ memory loss
Studies of post-mortem brains of NFL players who had neurological symptoms prior to death exhibited considerable loss of brain tissue, accompanied by enlargement of the cavities that produce cerebrospinal fluid (this fluid provides protection for the brain against mechanical and immunological injury), death of brain cells and build-up of brain proteins such as tau (rhymes with “pow”). The presence of tau in abnormal forms, or in places where it shouldn’t be, is a strong predictor of degenerative brain diseases such as dementia, including CTE and Alzheimer’s disease. What scientists are not completely clear on is whether tau plays a part in the brain degeneration or whether it is attempting to heal the damaged brain parts.
The first symptoms of CTE are a long period of mostly mood and
behavioral symptoms. The similarity of CTE symptoms to other
psychiatric disorders makes it hard to diagnose, thus, currently
CTE is confirmed post-mortem. 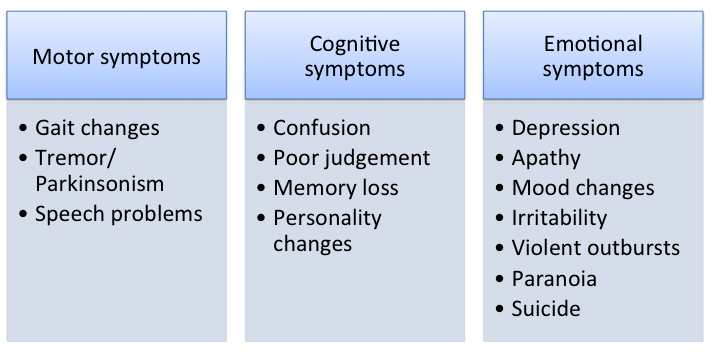
To make things a little more complicated, depression and cognitive problems (called post-concussive syndrome; symptoms like impaired memory, sleep disorders) are caused by multiple concussions and do not have to be associated with dementia development. Over half of people who suffer a single traumatic brain injury or multiple concussions are later diagnosed with major depressive disorder (symptoms include: Fatigue, impaired concentration, sleep problems, diminished interest or pleasure in almost all activities nearly every day, suicidal thoughts).
Concussion complications like dementia signal the end of the game for most people, with significant lowering of quality of life for decades. With efforts to understand what happens in the brain during a concussion, what causes the long-term problems of multiple concussions, and what can be done to treat it, perhaps we can fight to help the young and aspiring sport stars of the future. Let's blow the whistle on dementia and depression. So, what do we know about concussion? I’m going to cover some of the top ideas in research currently.
Kick-off: What causes concussion?
“Float like a butterfly and sting like a bee.” - Muhammad Ali, boxing
The brain is able to move within the skull. Think of the way jelly (Jell-O) moves in a bowl. The biomechanical properties of the brain allow it to sustain a certain amount of force (such as walking, 1 G; roller coaster drop, 5 Gs) without causing damage to its structure. However, when the brain is “stung” (fast change, sudden acceleration or deceleration), the force defending properties are overcome causing brain damage.
A force propagating through the brain strong enough to cause concussion (thought to be 80 – 120 G) causes disconnection of brain networks. As a result, the brain stops communicating information effectively, contributing to the common symptoms of concussion, depression and dementia.
First quarter: Concussion is like a brain fracture
“With concussion, you haven’t got a cast on, you’re not on crutches and you’re not in a sling. People assume you’re fit to go. It’s frustrating because you’re trying to explain what’s going on.” – George North, Rugby
The brain is split into different areas with different functions. Brain networks consist of nerve fiber bundles connecting the different areas. The fiber bundles are called white matter tracts. If you liken the brain to a house, then each brain area is like a room. Each room in the house has a different function. The kitchen is for cooking, the bedroom for sleeping and the bathroom for showering. Each room has a different function, but together they make a home.
The white matter tract is analogous to the electrical cable bundles running through the house distributing electricity for things like lights. From time to time you can switch lights off in a room but the cable allows all of the rooms to function together. Areas of the brain with different functions that communicate towards a common goal need to be connected to perform tasks that require a lot of different information and energy, e.g. attention, problem solving.
Strong blows to the head, especially rotational, cause twisting, stretching and shearing damage to white matter tracts. Further concussions can lead to swelling, breaking and snapping that disconnects white matter tracts from their targets.
To put it bluntly, a concussion is a fracture of your brain communication cables.
Yikes. Sounds horrible, doesn’t it?
Communication signals from one brain area to another (particularly brain areas called the cortex and the thalamus) are now compromised and the brain fails to perform network functions such as attention, working memory, problem solving, being able to switch between tasks, and reasoning as easily. The damaged communication cables lose their contacts, or become less efficient, requiring more energy or more brain areas to perform the tasks.
Depending on the brain areas and networks that are disrupted in this manner, other problems like depression and dementia can appear. Depression, for instance, is associated with alterations in networks linking limbic, cortical, and subcortical brain regions (alongside neurochemicals in these areas).
Damage may also lead to neurodegenerative disorders like dementia, Alzheimer’s disease, Parkinson’s disease and ALS. Microtubules and neurofilament proteins, such as tau, help maintain the structure of white matter tracts, but the fractures may cause them to form tangles or plaques. When brain areas with specific functions, like memory, start to get tau tangles or even amyloid-β plaques, the function of that brain area is progressively diminished, resulting in dementia. Tangles of proteins, or plaques, tend to follow the pathways marked out by white matter tract connections so that seemingly unconnected, widespread areas of the brain can be affected. As I mentioned, at this point it is unknown whether tau is causal or trying to heal the brain in light of an injury.
Second Quarter: Concussion sends your brain into an energy crisis
“I was hoping he would get up so I could hit him again and keep him down.” - Mike Tyson, boxer
In addition to large white matter tract fractures, smaller connections between brain cells, called axons, also become stretched and damaged. Ions that regulate axon electricity conduction are pushed into overdrive, leading to increased electrical activity, promoting cell death. The brain cells then kind of short circuit, which leads to a shutdown of brain activity. The brain has mechanisms like a circuit breaker in your house to help protect the brain from further damage when the current gets too high. This spreads through the brain quickly and far apart brain areas are affected simultaneously leading to concussion symptoms, like amnesia and loss of consciousness.
All this (combined with diminished blood flow, increase glucose use by damaged brain cells, and a myriad of processes set into motion to try to fix broken axons and damaged brain cells) causes an energy crisis. Energy starved brain cells cannot perform at their peak. This increases the risk of detrimental effects of further concussions, with further axonal damage and risks of build-up of dementia-associated proteins, including tau and amyloid-β (Alzheimer’s disease).
Third Quarter: The brain fights concussion with an immune response
“Our brains are doing a weird thing, messing with our emotions, messing with our sensitivities. And that can drive a person mad.” John Jaso, Baseball
The first line of defense against damage to the brain and spinal cord caused by trauma (or infection) are a type of brain immune cell called microglia.
They act like a brain referee and respond very quickly to brain cells damaged by trauma and stuff crossing from the body to the brain because of a breakdown in the protective blood brain barrier. These responses are collectively known as inflammation. Inflammation is important for brain repair but there are also some negatives that can predispose the brain to further damage if the brain doesn’t fully recover.
Inflammation persists in the brain well after concussion and may progress with time. This “primed” inflammation system means that responses to further trauma (multiple concussions) can amplify and exaggerate future immune responses.
Normally microglia work to clean up injured cells and debris from injured parts of the brain. But, prolonged and exaggerated (chronic) inflammation can cause the brain to kind of turn on itself, contributing to further destruction and, in the case of multiple concussions, also lead to accumulation of tau. Basically, too much of a good thing can be a double-edged sword.
What’s most interesting is the fact that if the brain is on guard in this primed inflammation state, such as the case after a concussion, any kind of impact on the brain immune system, not limited to a physical trauma, might cause deleterious effects. This would include an infection or even stress.
So, concussion plus concussion; or concussion plus flu; or concussion plus exams… could lead to a greater risk of depression or dementia down the line.
Fourth Quarter: Multiple concussions knockout brain cells
“It's not whether you get knocked down; it's whether you get up.”- Vince Lombardi, American football
Everything I have discussed above can cause death of brain cells. Multiple concussions lead to brain shrinkage, mainly due to loss of brain cells and connections between brain cells. This is called atrophy. Areas of the brain that lose brain cells include the amygdala (emotion), hippocampus (memory), cortex (attention, problem solving), and cerebellum (balance).
Loss of brain cells is dominant to progress of symptoms in neurodegenerative diseases like Alzheimer’s disease, Parkinson’s disease, ALS and the sports-related dementia called CTE. Cortical thinning is one of the most sensitive markers of brain degeneration. It can be measured in patients using non-invasive brain scanning techniques early in the progression of brain damage.
Here’s what is scary: cortical thinning is not only present in older professional athletes, but also in young athletes and children with a history of multiple concussions.
The Anderson lab at University of Arizona, has been tackling the problem of repetitive brain injury on developing brains. Using rodent models, they have found that young brains subjected to multiple concussions already show considerable cortical thinning with loss of brain cells. Indeed, in other labs, brain scan studies in young athletes found cortical thinning (in cortical areas associated with dementia, other cognitive impairments and emotion regulation), with increasing severity with the number of concussions.
This suggests that multiple concussions in young brains can set into motion brain changes to make them more prone to dementia and depression later in life. The effects of concussion on the brain during childhood are particularly important as any disruption of normal brain function, when the brain is still developing, can impact many aspects of a child’s life and, importantly, last a lifetime.
Unfortunately, studies in young brains are limited. Many believe that youth is a period of indestructibility but young brains are more vulnerable to concussion than adult brains. They are more susceptible to injury, the progression of the brain trauma is different and recovery is longer. This is due to differences in the amount of fluid surrounding your brain, how well formed the barrier between your brain and the blood stream is, how well the white matter tracts are insulated and differences in elastic properties.
Importantly, especially for our youth, brain atrophy is measurable while the injured person is still alive and these brain changes are associated with changes in cognitive abilities can also be measured (like verbal fluency). Being able to identify and measure concussion will help identify those who need treatment and possibly stop deleterious long-term problems in their tracks.
Time out: treating a concussion with rest
“Lads, you're not to miss practice unless your parents died or you died.” - Frank Leahy, American football
Guidelines state that the most important thing to do if you have concussion is REST. This includes physical (no sports etc.; “return to play”) and mental exertion (no school/ work, homework, screens, computer games; “return to learn”). It’s advised that brain rest is implemented for as long as it takes for all concussion related symptoms to be alleviated. Sticking to the instructions for recovery is not quite as easy as donning a cast for a broken bone, especially for kids. However, more research is required to better understand what is best for the brain post-concussion and what return to play/ return to learn guidelines should be. See box “Towards better sport concussion management”.
Instant Replay: Attacking concussion head on
“… you can try to build all the helmets you want to build, but if you have two guys at 220 pounds each and they’re running into each other at 25 or 30 miles an hour that’s like a car accident. There’s going to be some trauma there no matter what kind of equipment you’re wearing.” - Dave Scatchard, Ice Hockey
The best way to tackle concussion in sports is to minimize the risk of head injuries, for instance, not heading the ball in soccer, or using proper protective gear (although some suggest that this makes athletes more prone to injury due to perceived protection leading to greater risk taking).
It is hard to diagnose concussion because symptoms can depend on age, gender, history of injuries, and, reluctance of athletes to report their symptoms in fear of being removed from the game and not being able to compete. Concussion behavioral symptoms can improve a long time before the brain has finished repairing itself.
With the risk of brain injury coming to a head in sports due to increased awareness, a number of things are coming into play to study and identify concussion in a more objective manner:
- Technology to measure concussion in real time. Helmets reduce concussion but do not prevent them. However, “smart" helmets and mouth guards have been designed to measure the force of impacts during games to help determine who and when people get concussion. It seems that the best indicator of a concussion is a blow to the top of the head… where, ironically, most helmets do not protect.
- Biomarkers in the blood stream or brain fluid can predict concussion severity or neurological disorders. These biomarkers measure levels of white matter tract injury, neuroinflammation markers, tau and neurofibrillary tangles.
- Neuroimaging brain scans e.g. MRI, fMRI, EEG, Diffusion Tensor MRI
- Behavioral and neuropsychological tests
Closing commentary: a-head of the game for our young
"I have headed the ball so many times. I have walked the road. I want to make sure that I give the kids the right information and educate them so that they can live a happier, healthier, longer life than me." – Abby Wambach, Soccer
Sport and exercise is valuable for a number of reasons, both physiologically and psychologically. We don’t want to create a culture of fear of sport. However, we owe it to the younger generation to take heed of what we know about the damage concussions can do to the brain for a lifetime, to minimize the risk of concussions and to treat the brain adequately with rest before returning to a game or school.

The highest risk of concussion for boys is American football and for girls is soccer. Interestingly, girls suffer a higher rate of concussion than boys in similar sports (perhaps because of weaker necks, smaller head mass, or that they are more likely to report symptoms than boys).
Concussion in sports is preventable. However, in case of prevention failure, every athlete, young and experienced, should be prepared to recognize the signs of a brain injury, to speak up and not cover up their brain injury, and be given appropriate time to recover.
Athletes, coaches, parents, medical professionals and fans must make headway to discourage the glorification of getting up and continuing to play despite “seeing stars”.
Use your head. No win, no trophy, no gold medal and no scholarship should come with the cost of a lifetime of living with a brain that doesn’t work properly.
Reading list
Useful/ interesting websites:
https://www.headway.org.uk/
http://www.ninds.nih.gov/disorders/tbi/tbi.htm
http://www.cdc.gov/traumaticbraininjury/get_the_facts.html
http://www.aans.org/Patient%20Information/Conditions%20and%20Treatments/Sports-Related%20Head%20Injury.aspx
http://playerwelfare.worldrugby.org/concussion
http://usarugby.org/concussions
http://www.englandrugby.com/my-rugby/players/player-health/concussion-headcase/management-of-concussion/
http://playerwelfare.worldrugby.org/concussion
http://www.pbs.org/wgbh/pages/frontline/concussion-watch/
https://en.wikipedia.org/wiki/List_of_NFL_players_with_chronic_traumatic_encephalopathy
Infographics:
http://www.evanshealthlab.com/concussion-the-first-week-infographic/
http://visual.ly/your-brain-concussion
http://www.chop.edu/health-resources/what-are-symptoms-concussion#.VjWrjLwd6u4
The Blog was written by Carolyn Lacey, Scientific Outreach Manager at Neurexpert. To learn more about Carolyn and Neurexpert, please click here.
Special thanks to Trent Anderson, The University of Arizona, for answering many questions.
Recent Blog Posts
What connects schizophrenia and autism?
On the surface, many brain disorders appear to be quite different. It’s not often that you hear of someone with, say, depression being compared to someone with schizophrenia or, indeed, Autism Spectrum Disorder (autism). However, if you dig deeper and break down the symptoms you will find that they share some commonalities: altered social interaction; impaired cognitive function; memory impairment; tendency towards compulsive behavior; attention deficits; and abnormal sensory processing.
Want to rid your brain of toxic build-up and perhaps stave off Alzheimer’s Disease? Don’t sleep sitting up
Planning on taking a power nap at your desk today? You might want to think twice about your sleeping position. The research article I’m about to summarize makes me think of all those times I have actually managed to get some sleep on a long-haul flight… only to wake up still feeling terrible (even after drinking litres of water) and all the elderly people I know who often like to take cat-naps sitting in their favorite armchairs.
What has birth got to do with autism?
A prominent neuroscientist suggests that the trend towards greater birth interventions could be correlated with greater incidence of autism spectrum disorders. We discuss his reasoning in our latest blog post.
Sleepless with the Enemy: how skipping sleep changes your social life and how dreams become reality
Ever stay up too late and wake up thinking the world is out to get you? We cover a new study that shows that sleeping and dreaming helps you read other people better. Skipping just one night of sleep makes your brain read threat in friendly faces and, in contrast, bigger dreams make for better reality.
Depressed? Suck it up!
Depression sucks and anti-depressants often don't work. Our latest blog sniffs out a new treatment published in Molecular Psychiatry that could be the future for #depression sufferers.
Stressed out of my mind
June 27th is Post-Traumatic Stress Disorder (PTSD) Awareness Day and so this blog is dedicated to neuroscience related to chronic stress.
Exciting times ahead at Neurexpert
Neurexpert appoints Dr Carolyn Lacey as Scientific Outreach Manager

Brochure Publications